A vital tool for maintaining our health or a looming threat? Why not both? What is inflammation, and what can we do when it gets out of control?
Inflammation accompanies us throughout our lives. In fact, it is so common that in everyday speech the word “inflammation” has almost become synonymous with disease, such as arthritis (joints inflammation), urinary tract infections (inflammatory conditions), skin inflammation, lung inflammation, liver inflammation, gastrointestinal inflammation, and so on and so forth. Inflammation is typically portrayed as something burning, fiery, reddish, and negative. But how can inflammation also serve a beneficial process?
In fact, inflammation is not a “disease”. Not in the conventional sense. Under normal circumstances, inflammation is an immune response that aims to protect the body from foreign elements. This response can be triggered by exposure to bacteria, viruses or parasites, but may also be due to physical damage sustained by tissues following penetration of the body by a foreign object, such as a thorn. We only notice inflammation that has developed in a wound when it is already infected by bacteria, red and swollen. However, the inflammatory process begins much earlier, when the immune system tries to fight off the harmful invader.
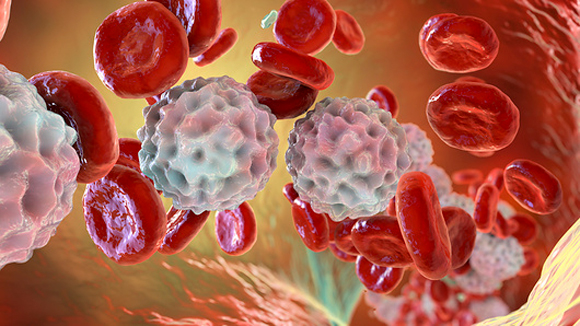
White blood cells in the blood stream | Kateryna Kon, Science Photo Library
How It Happens
Many factors can elicit an inflammatory response in the body, including exposure to bacteria, viruses or parasites, as well as a scratch or injury that breaks the skin barrier that protects our body, thus exposing us indirectly to bacteria. Furthermore, even non-routine factors, such as harmful radiation or dangerous substances, may lead to the development of inflammation in the body.
The main cgaracteristics of inflammation include redness, a rise in body temeprature, pain and swelling. Many cells of the immune system are involved in the inflammaroty process. Among other things, they release substances termed 'Inflammatory mediators'.
Two of these are the hormones, bradykinin, and histamine, that cause the small blood vessels in the tissue to expand and allow more blood to reach the damaged tissue. This is the source of redness in the inflamed region, as well as the feeling that it is hotter than its surroundings. The elevated blood flow allows more white blood cells from the immune system to reach the damaged tissue and aid the healing process. These two hormones also stimulate the sensory nerves and cause them to send pain signals to the brain. It is thought that the feeling of pain has a protective function: if the damaged organ hurts, we’ll be careful not to put it in danger in the future.
Inflammatory mediators have another job: they make it easier for the white blood cells to cross the walls of the small blood vessels and penetrate the damaged tissue. These cells also increase the infiltration of fluids into the inflamed tissue, thus sometimes leading to swelling. Moreover, cells from the mucous membranes tend to release more fluids to their surroundings during inflammation. This happens, for example, when the nose is blocked and the membranes lining it are inflamed. The large amounts of fluid in the inflamed area probably help to rapidly flush out the foreign elements.
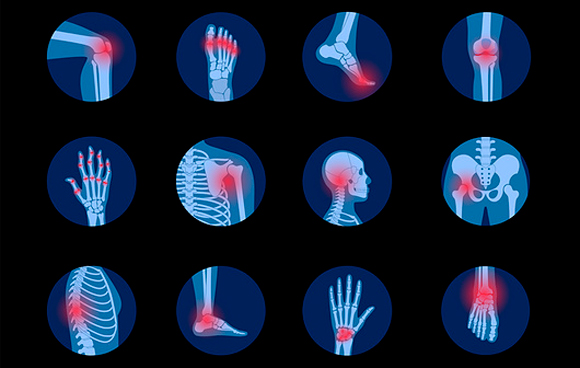
One manifestation of inflammation is chronic inflammation that causes pain and stiffness of the joints. Rheumatoid arthritis | Illustration: Pikovit, Science Photo Library
Types of Inflammation
Inflammation can manifest in many ways. The first is acute inflammation, which stems from tissue damage following trauma, infection by bacteria and other pathogens, or exposure to harmful compounds. This type of inflammation spreads rapidly and may escalate within a short period of time. Nonetheless, it usually also subsides relatively quickly and its symptoms generally last only a few days.
In contrast, chronic inflammation is a slow, long-term inflammation that develops as a result of external or internal factors and is characterized by the accumulation and activation of immune cells and damage to body tissues due to prolonged inflammatory response. Prolonged inflammation may last for several months or even years and its extent and impact vary according to the cause of the injury and the body’s ability to repair the damage.
Although chronic inflammation develops quietly, without ongoing traumatic events, it is present in most chronic diseases and threatens the health, quality of life, and life expectancy of those who suffer from it. While the role of inflammation is to help the body, sometimes it can actually cause harm. When the immune system operates continuously and for an extended period of time, the side effects of its activity can be destructive. In other cases, prolonged release of proinflammatory substances damages body tissues and can sometimes contribute to the development of autoimmune diseases, in which the immune system attacks the body’s own cells and tissues.
Chronic inflammation is considered to be a main contributor to the development of heart disease, diabetes, autoimmune diseases such as rheumatoid arthritis, allergies, and even cancer.
Chronic inflammation is not an actual disease, but rather a process that involves prolonged activation of immune cells. Chronic inflammation is associated with multiple and diverse diseases—such as cardiovascular diseases, diabetes, malignant diseases, autoimmune diseases, chronic liver and kidney disease, and more. In order to confirm or rule out the presence of a chronic inflammatory situation it is necessary to examine the patient’s medical history and perform both a physical examination and routine laboratory tests. In some cases doctors also request other relevant tests for diagnostic purposes. For example, colonoscopy, a test during which a tiny camera is inserted into the intestines via the anus, can assist in the diagnosis of inflammatory bowel disease.
Finally, when inflammation develops without any apparent reason, and there’s no sign of infection or injury, it is referred to as sterile inflammation. In such cases, it seems that the immune cells mistakenly identify proteins or molecules of the body cells as foreign elements and act against them. Such a response may be elicited, for example, by substances released from a tissue with necrosis or uncontrolled cell death. The incorrect identification leads to the activation of the immune system and to an inflammatory response.
Pharmacological Treatment aimed at reducing the activity of proinflammatory agents. Anti-inflammatory tablets and capsules | FOTOGRIN, Shutterstock
Drug Treatment
Anti-inflammatory medication usually aims to directly or indirectly reduce the activity of the immune system and suppress the action of inflammatory mediators. Many of the medications act to alleviate pain, reduce swelling, and often also prevent or slow down the inflammatory process.
Nonsteroidal anti-inflammatory drugs (NSAIDS), such as aspirin, ibuprofen or naproxen, act to halt the production of prostaglandins—molecules that stimulate many processes in the body, including inflammatory processes. In contrast, corticosteroids—such as prednisone—affect the activity of the genes involved in processes characteristic of chronic inflammatory diseases.
Complicated cases are sometimes treated with biological drugs, which are based on antibodies that can bind to specific cells in the immune system and limit their activity. These drugs can also be used to treat cancer and inflammatory bowel disease, or to prevent organ rejection after transplantation due to attack of the transplanted organ by the immune system.
Finally, chemotherapy drugs against cancer affect the ability of the body cells to divide. Since they also affect the division of immune cells, in other words, the ability to produce new cells, in some cases they can also be used to treat chronic inflammation. In such cases the drugs are administered at a low doses to minimize their typically severe side effects.

In most studies, high consumption of fruit, vegetables, legumes, and grains has been associated with lower inflammatory indicators, compared to a Northern European or North American diet. The Mediterranean diet. | gorillaimages, Shutterstock
Lifestyle Changes
In addition to, or as an alternative to, pharmacological treatment of inflammation, patients are often advised to adopt new habits, such as dietary changes and increased physical activity. Yet, the advantages of these can vary.
To examine the relationship between nutrition and inflammation, study participants are usually given questionnaires that assess their dietary habits and compare the responses to the level of inflammatory markers found in their blood. Most studies have shown that nutrition has a modest impact at best on changes in participants' inflammatory markers.
Changes in inflammatory markets, if any, have usually been observed following consumption of foods low in sugar, saturated fat, and trans-fats, and rich in dietary fiber, magnesium, carotenoids (organic pigments mainly found in plants), and flavonoids (compounds present in fruits and vegetables), which are also known as antioxidants. In most studies, the Mediterranean diet, which is characterized by the consumption of many fruits, vegetables, legumes, and grains, was associated with lower levels of inflammation compared to a Northern European or North American diet.
Regular physical activity at moderate intensity contributes greatly to controlling the activity of the immune system and moderating inflammation and chronic disease. Studies have shown that numerous mechanisms are involved in the anti-inflammatory effect of physical activity. During physical activity the body increases the production of adrenaline, cortisol, growth hormones, and prolactin, which are all involved in the activity of immune cells and in their distribution throughout the body.
Regular physical activity also burns some of the body’s fat stores. Our body contains two types of adipose tissue (fat): white and brown. Excess white adipose tissue contributes to the production of pro-inflammatory mediators in the body, so burning fat to produce energy during physical activity makes it easier for us to regulate inflammatory processes.
The activation of skeletal muscles during physical activity contributes to the fight against inflammation. It causes the cells to release substances that contribute to metabolic processes, increasing the absorption of sugars and fats, thereby reducing the risk of metabolic disorders and of the development of inflammation. Moreover, it has been found that people who do little physical activity have an increased activity of pro-inflammatory receptors in cells of the immune system. This increase is also related to the development of chronic diseases and inflammation. Conversely, physical activity reduces the presence of these receptors on the cell surface.
While the word “inflammation” often evokes negative associations, a regulated inflammatory response is essential for maintaining our overall health. Without it we would have difficulty warding off external threats and foreign invaders in our body and would be susceptible to diseases and infections. However, when this delicate balance is disturbed, and the immune system becomes overactive, the inflammatory process can harm our cells and tissues. So the next time you sustain an injury, observe the reddened, swollen and sore wound and appreciate your immune system for performing its job faithfully.
